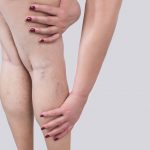
Dealing With Varicose Veins Before, During and After Pregnancy
 During pregnancy, your body’s blood volume increases significantly to prepare for the amount of blood lost during childbirth. This circulation change is designed to support your growing baby, but unfortunately, it can also lead to bulging, painful veins.
While varicose veins are not an attractive attribute, they do not pose a significant health risk to you or your baby. They can, however, cause discomfort, swelling, and in worse cases, blood clotting. Treatments for removing varicose veins are rarely performed during pregnancy, so here’s how to manage them before, during, and after pregnancy.
During pregnancy, your body’s blood volume increases significantly to prepare for the amount of blood lost during childbirth. This circulation change is designed to support your growing baby, but unfortunately, it can also lead to bulging, painful veins.
While varicose veins are not an attractive attribute, they do not pose a significant health risk to you or your baby. They can, however, cause discomfort, swelling, and in worse cases, blood clotting. Treatments for removing varicose veins are rarely performed during pregnancy, so here’s how to manage them before, during, and after pregnancy.
How Pregnancy Can Cause Varicose Veins
Varicose veins are large, swollen blood vessels commonly found in the legs, but they can also occur almost anywhere in the lower body during pregnancy. Varicose veins create a distinctive purplish bulge above the skin, and while they look alarming, they’re relatively harmless. Fairly common, approximately 20% of women experience them during pregnancy. The extra volume of blood produced during pregnancy puts extra pressure on your blood vessels, especially the veins in the legs. The veins in your legs have to work against gravity to push all the extra blood back to your heart, and during pregnancy, there is extra pressure on your pelvic veins. This extra blood and pressure can cause the valves in the veins to malfunction, thus causing varicose veins.How To Find Relief During All Stages of Pregnancy
While pregnant, there are several things you can do to minimize varicose veins and keep them under control. You can reduce the amount of time spent on your feet and elevate your legs when possible. There are no surefire ways to prevent varicose veins, but these tips may help you find relief from varicose vein discomfort during all stages of pregnancy. If varicose veins do pop up, the key is to keep your blood moving. These tricks can help you keep your varicose veins under control:- Cut back on the hours you spend standing or sitting. Believe it or not, both sitting and standing can lead to varicose veins. Light exercise that keeps your legs moving helps prevent blood from pooling up. Try to get up and get moving every 30 minutes or so.
- Wear compression stockings to manage the symptoms. There are full-length pregnancy versions that go higher than the calf and are especially helpful in the vulvar region — and they look like nylons so that nobody will be the wiser. But they are pricey. Bike shorts provide similar compression in that area at a more affordable price.
- Try different positions to reduce pain and other symptoms. Lay on your left side to take the pressure off your main blood vessels. Elevate your legs above your heart to help your veins circulate blood. Avoid sitting cross-legged, which increases the pressure on your legs.
Varicose Vein Risk Factors During Pregnancy
Of all the risk factors for varicose veins disease, pregnancy is one of the highest risk factors for chronic venous insufficiency. Other factors include hereditary and standing on feet for long periods. If you have all three risk factors, then you are at very high risk. Those with varicose veins during pregnancy routinely need ultrasounds during pregnancy to rule out problems, such as large veins and stagnant flow that can occur and afflict those patients with vein disease. Thrombophlebitis and blood clots can occur in veins and can be heightened during pregnancy. An ultrasound can rule these out and predicate a treatment algorithm.Managing Varicose Vein Pain While Pregnant
Along with compression stockings, you can do several other things to help with the discomfort and pain caused by leg veins. During pregnancy, the uterus exerts pressure on the inferior vena cava. This vein is responsible for transporting blood from the legs and feet to the heart. If the vena cava is restricted in some way, blood will pool in the feet and legs, leading to varicose veins. This is why your OB/GYN likely advised you to lie on your left side when resting or sleeping, as it prevents excess pressure on this vein. Drinking plenty of water can also help your body maintain a proper fluid balance. Other options for managing varicose veins during pregnancy include maintaining the weight recommended by your OB/GYN and avoiding long periods of sitting or standing. If your veins continue to bother you after you have given birth, you will benefit from ultrasound and evaluation with a Vein Specialist.Treatment Options After Pregnancy
Although varicose veins that develop during pregnancy often resolve on their own after giving birth, some patients will require treatment. In these cases, we offer treatments for venous disease that are non-surgical and performed in our office in less than an hour. To learn more about the vein treatment options we offer in the La Porte area, contact Vein & Laser Institute to schedule a consultation.Recent Posts